The EMDR app: First third-party app with Assistive Access
Digital bilateral stimulation is now accessible to users with cognitive and motor disabilities.
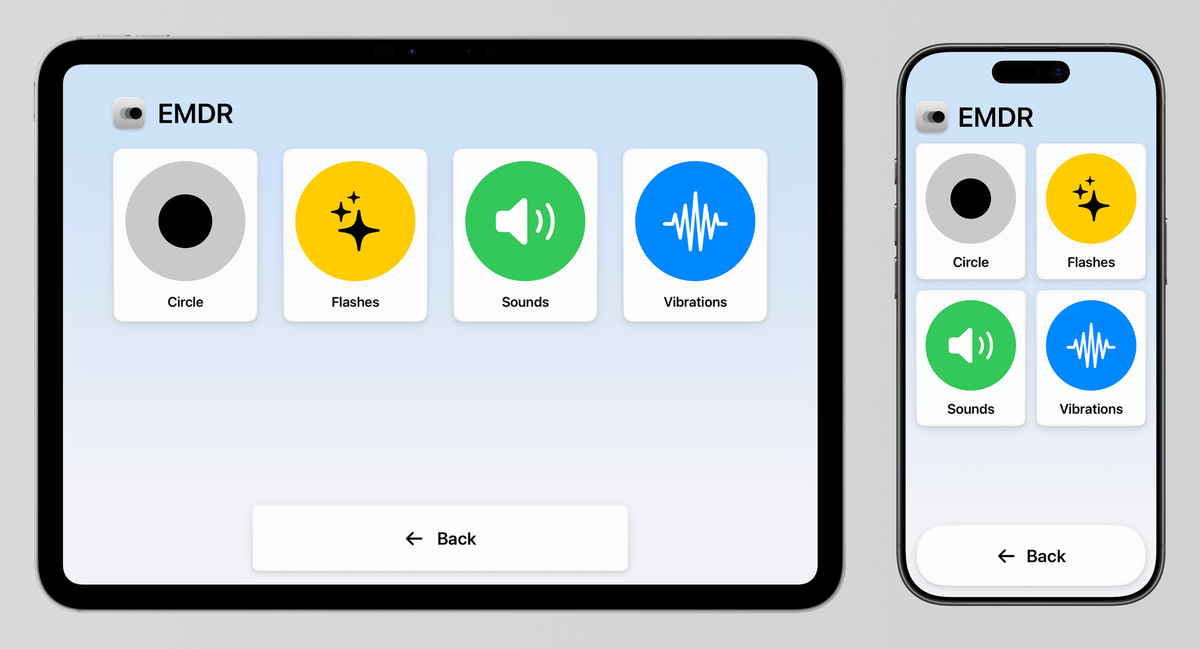
With the latest update, the EMDR app becomes, to our knowledge, the first third-party application to ship a dedicated interface for Apple’s Assistive Access. This advancement reflects our commitment to building digital mental health tools that are both inclusive and ethically responsible.
Assistive Access is Apple’s simplified mode for iPhone and iPad, for people who find conventional smartphone interfaces overwhelming or difficult to navigate. It reduces visual complexity, enlarges interactive elements, and limits the interface to a focused set of functions with predictable navigation. Apple introduced the feature in 2023 but only recently provided the APIs necessary for third-party developers to build for it. To date, no third-party app, therapeutic or otherwise, has done so.
Why accessibility matters in a therapeutic context
The EMDR app provides visual, auditory and haptic bilateral stimulation, used by therapists and clients within EMDR therapy contexts. During a session, attention should remain on the therapeutic task rather than on operating the technology itself. This holds for any user, as complex interfaces or multi-step settings can interrupt the flow of a session.
The standard EMDR app interface already prioritizes simplicity. Designing for Assistive Access required us to go further: we had to identify the essential functions and remove everything else. The result is an interface reduced to its clinical core: select a stimulation modality, adjust the tempo, and begin the session.
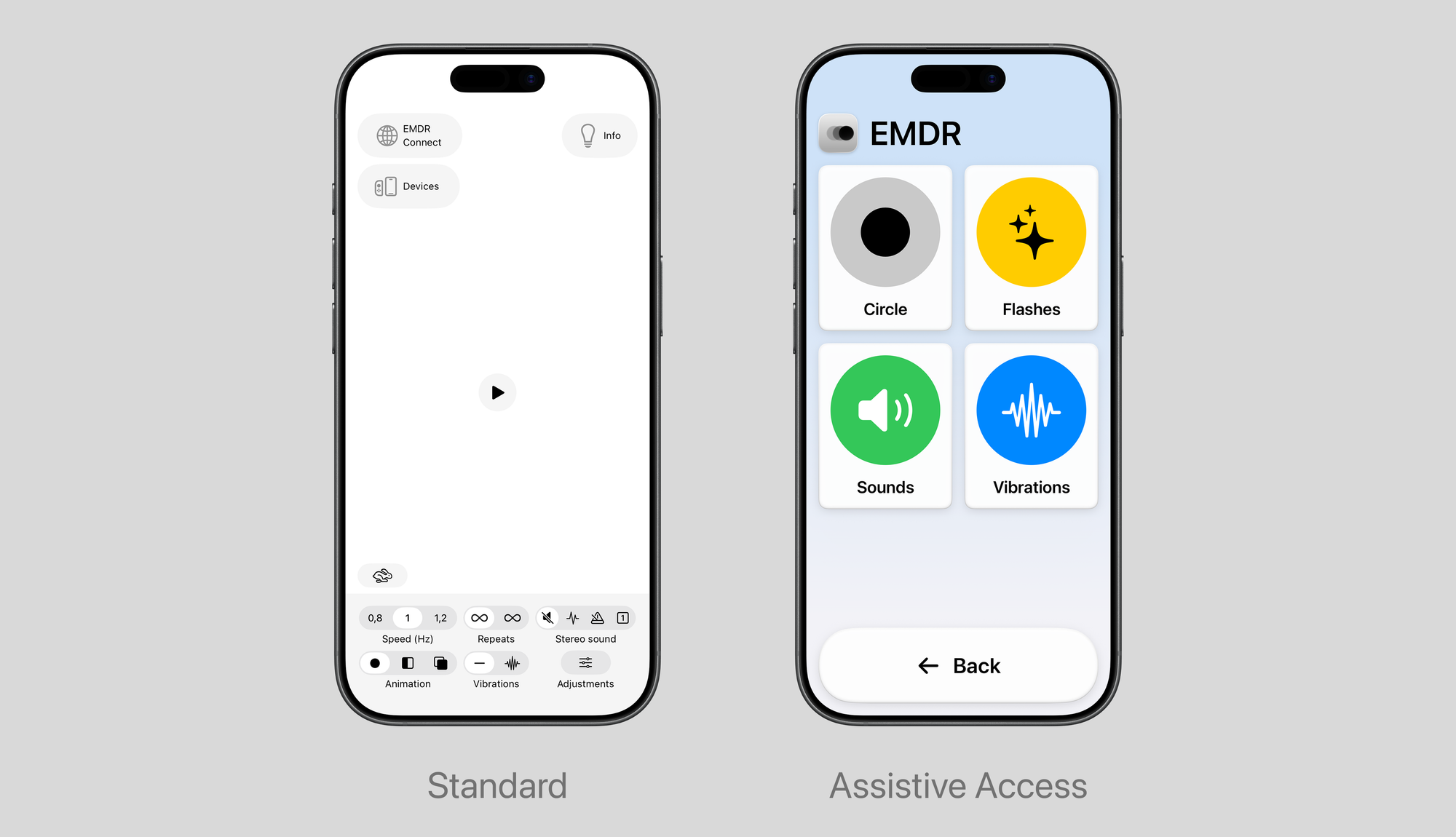
Who this feature is for
The Assistive Access interface was designed with specific populations in mind. We focused on individuals with cognitive and motor impairments, visual limitations, or lower digital literacy, as well as people experiencing acute stress or anxiety, where complex interfaces can become an additional burden.
The last group deserves emphasis. Accessibility is not only relevant for permanent disabilities. Fatigue, psychological distress and cognitive overload can also make interacting with any technology more challenging. A therapeutic app, that's used precisely in moments of psychological vulnerability, should be designed with this in mind.
The design process
We developed the Assistive Access interface by following the CeHRes Roadmap (Van Gemert-Pijnen et al., 2011) and the Person-Based Approach (Yardley et al., 2015), both established frameworks for digital health intervention development. We began with mapping the needs of users with cognitive, motor, or visual impairments, individuals with different levels of digital experience, and therapists who use the app in practice. We translated our findings into three guiding principles:
The user feels empowered to use the app without difficulty. User goals are completable with minimal interaction. Through clarity, predictability and error tolerance, users who normally need support can preserve independence and autonomy.
Cognitive load remains low, while clinical effectiveness is preserved. The interface only includes clinically relevant functions for bilateral stimulation sessions: stimulation modality and speed. These choices can optionally be enabled or disabled before entering Assistive Access, to account for user capability.
The app must be responsible in taking care of its users. We take great care in ensuring a focused experience by default, while further user specific adjustments can be set before enabling Assistive Access.
These principles were informed by research on interface design for cognitive disabilities (Amouzadeh et al., 2025; Minh, 2023; Ribeiro et al., 2024; Zhou et al., 2020) and on EMDR treatment adaptations for individuals with intellectual disabilities and dementia (Ruisch et al., 2023; Schipper-Eindhoven et al., 2024).

A gap that should not exist
No other therapeutic app and, as far as we can determine, no other third-party app of any kind is currently optimized for Assistive Access. Across the landscape of digital EMDR tools, accessibility features are consistently absent. This is not a minor oversight. All kinds of people can experience trauma. The extent to which digital mental health apps are optimized for the user’s diverse needs directly influences how the intervention is experienced and used.
We hope that this step encourages other developers in the digital mental health space to consider Assistive Access, and accessibility in general, as an integral part of responsible development, not as an afterthought. Making therapeutic technology usable for a wider range of people is more than an optional enhancement: it is a clinical and ethical obligation.
By Helena Zechner and Bas Oppenheim
Links
References
Amouzadeh, E., Dianat, I., Faradmal, J., & Babamiri, M. (2025). Optimizing mobile app design for older adults: systematic review of age-friendly design. Aging Clinical and Experimental Research, 37(1), 248. https://doi.org/10.1007/s40520-025-03157-7
Minh, V. N. (2023). Touch-screen application’s design guidelines for older adults with dementia. https://essay.utwente.nl/fileshare/file/95898/Vo_BA_EEMCS.pdf
Ribeiro, D. M., Melo, F. V., Negromonte, V., Matias, G. W., Farias, A., Azul, C., Chaves, A. P., & Gama, K. (2024). A Comparative Study on Accessibility for Autistic Individuals with Urban Mobility Apps. arXiv (Cornell University). https://doi.org/10.48550/arxiv.2410.14033
Ruisch, J. E., Nederstigt, A. H. M., van der Vorst, A., Boersma, S. N., Vink, M. T., Hoeboer, C. M., Olff, M., & Sobczak, S. (2023). Treatment of post-traumatic stress disorder in people with dementia: a structured literature review. Psychogeriatrics : the official journal of the Japanese Psychogeriatric Society, 23(3), 523–534. https://doi.org/10.1111/psyg.12951
Schipper-Eindhoven, S. M., De Knegt, N. C., Mevissen, L., Van Loon, J., De Vries, R., Zhuniq, M., & Bekker, M. H. J. (2024). EMDR treatment for people with intellectual disabilities: a systematic review about difficulties and adaptations. Frontiers in Psychiatry, 14, 1328310. https://doi.org/10.3389/fpsyt.2023.1328310
Van Gemert-Pijnen, J. E., Nijland, N., Van Limburg, M., Ossebaard, H. C., Kelders, S. M., Eysenbach, G., & Seydel, E. R. (2011). A holistic framework to improve the uptake and impact of eHealth technologies. Journal of Medical Internet Research, 13(4), e111. https://doi.org/10.2196/jmir.1672
Yardley, L., Morrison, L., Bradbury, K., & Muller, I. (2015). The Person-Based Approach to Intervention Development: Application to Digital Health-Related Behavior Change Interventions. Journal of Medical Internet Research, 17(1), e30. https://doi.org/10.2196/jmir.4055
Zhou, L., Saptono, A., Setiawan, I. M. A., & Parmanto, B. (2020). Making Self-Management Mobile health apps accessible to people with Disabilities: Qualitative Single-Subject study. JMIR Mhealth and Uhealth, 8(1), e15060. https://doi.org/10.2196/15060

